Empathy
"But He Was Drunk": Judging Our Patients
A Personal Perspective: How easily we can lose our empathy for one another.
Posted August 8, 2023 Reviewed by Michelle Quirk
Key points
- It's common in health care to make uncharitable judgments about our patients.
- It's common in society to be judgmental about those less fortunate than us.
- Loss of empathy is a cardinal sign of burnout.
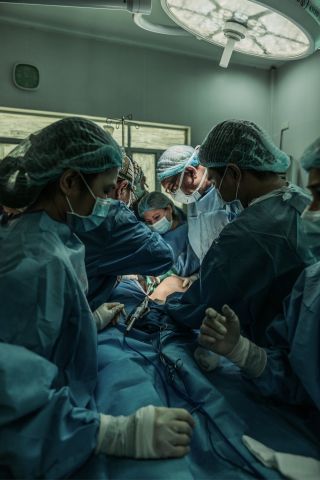
Through the decades, I must have made several thousand trips down to the trauma bays of my various medical centers to see one terribly injured individual after another. Every time, they would be surrounded by a dozen caregivers assessing and tending to their injuries. When I would enter the room, one of the team would always turn to me and give an account of the accident that resulted in the patient’s injuries.
It always seemed to involve some Rube Goldberg sequence of events resulting in the victim being thrown through something, chewed up by something, impaled by something, or smashed into something. The stomach-turning tale would always be followed by a rundown of the many bones, organs, and soft tissues that had been torn, sliced, pulped, or shattered.
But, He Was Drunk.
Then, the reporting agent would finish up with a familiar coda: “But, he was drunk!”
Or, he was high, or texting, or going the wrong way down a one-way street, or ignoring posted warnings, or shooting up, or running from the police. One way or the other, such a tagline, and a theatrical roll of the eyes, was compulsively addended to the overall assessment. As if it explained everything. As if without said ill behavior, this episode of the cosmos gratuitously unloading on some unfortunate soul would have never occurred. As if, had said soul been minding his own business and following the straight and narrow, he would not have come to such a fate. As if, somehow, he deserved this fate—that the universe was, indeed, righteous in its action.
Near Miss
And hearing this, I would always be transported back to one Saturday night during my youth. The guys and I had crammed into my friend Pat’s VW Rabbit and crossed the Delaware to visit another friend, Chris, at Lafayette College. Chris greeted us with several bottles of rot-gut bourbon and ordered us to drink—in commiseration with his broken heart. His longtime girlfriend had just given him the heave-ho.
We offered little resistance, but when faced with the prospect of having to sleep in his fraternity’s basement, we decided to head back to New Jersey and “crash” at Pat’s farmhouse. Only, being responsible former members of the National Honor Society, we all admitted to being too tipsy to drive. Until one of the group stepped forward, grabbed the keys, and proclaimed, “No worries, guys; I’m fine.”
I’m happy to report that we made it back to the farmhouse without incident. The next morning, however, Pat enquired as to who actually drove us home. I responded, “That would be me.” He motioned for me to come look out his living room’s large picture window. There, a set of tire tracks zig-zagged across his sizable front lawn and through the front vegetable garden, leading to the Rabbit, sandwiched into a row of azaleas by the front steps.

My point here is that I, and my buddies, could have easily ended up laid out in a trauma bay that night because of our (my) drunken stupidity. And every time I think about it, I have to ask myself, had we ended up so, would we have been any less deserving of good care? Of professionalism? Of compassion? Had we checked our right to sympathy at the car doors that night? Were we all lesser beings because of our moronic actions? I would argue, no.
Do We Judge the Worthiness of Our Patients?

So what’s behind this reflexive denigration of the horribly injured who pass so frequently through our doors? Or, for that matter, of so many of the other patients we encounter? Consider how we view the heart attack patient—“Figures, he’s never exercised a day in his life”; the diabetic – “Well, of course her sugar’s out of control; look how obese she is”; the cancer patient—"What does he expect, after smoking his whole life?”
Is it a defense mechanism against secondary traumatization? Do we engage in it to continue our jobs without becoming paralyzed by the arbitrary nature of the universe? By the realization that tragedy and mayhem could befall any of us, or someone we love? Would admission to the sheer randomness of cataclysmic happenstance be too much for us to bear, to press on in our grim work?
Or, do we need to feel superior to the afflicted for some reason? Do we search for something, anything, to tell ourselves that we are better than them, that “they” are different from “us"? Is it a sign of the depersonalization of burnout—a loss of empathy?
Is Care Affected by Our Opinions of Our Patients?
And here’s the rub: What happens when some sympathy, some empathy, some compassion is subtracted from our care? Does it give us an excuse not to go all in, not to be quite as vigilant, not to demand the very best out of ourselves? Does it affect how we interact with patients and their families? Does it influence how those around us are treating them? Could it affect our decision-making and our patients’ outcomes?
Not Just Health Care Providers

In fact, aren't we all prone to doing something similar? Don't we often assume the worst with those who are beset by misfortune? Those whose lot in life is not as rosy as ours? Those whose decision-making has been chronically askew?
Empathy is such a critical factor in adaptive human interactions of all kinds and, ultimately, in maintaining our own well-being. Its loss is a warning sign for burnout. Might it be best to stow away our judgments and seek to amp up our empathy? Even in the most judgment-precipitating situations with the most judgment-precipitating of people? I venture that it would certainly be of benefit in the hospital. But, goodness knows, a little more “there but for the grace of god go I” might go a long way in our ever more divisive society.
References
Mottaghi,S., Poursheikhali,H., Shameli,L. Empathy, compassion fatigue, guilt and secondary traumatic stress in nurses. Nurs Ethics. 2020 Mar;27(2):494–504.doi: 10.1177/0969733019851548. Epub 2019 Jul 8. PMID: 31284826
Cocker,F., Joss, N. Compassion Fatigue among Healthcare, Emergency and Community Service Workers: A Systematic Review. Int J Environ Res Public Health 2016 Jun 22;13(6):618. doi: 10.3390/ijerph13060618. PMID: 27338436
Woo, M., Kim, D. Factors Associated With Secondary Traumatic Stress Among Nurses in Regional Trauma Centers in South Korea: A Descriptive Correlational Study. J Emerg Nurs 2021 May;47(3):400–411. doi: 10.1016/j.jen.2020.08.006. Epub 2020 Nov 21. PMID: 33229000
Simonds, G., & Sotile, W. (2019). Thriving in Healthcare. Huron Consulting Group LLC. ISBN-10: 1622181085
Simonds,G., Sotile,W. (2018) The Thriving Physician: How to Avoid Burnout by Choosing Resilience Throughout Your Medical Career. Huron Consulting Group, ISBN-10 1622181018




