Chronic Pain
Understanding the Psychology in Chronic Pain
Why pain psychology treatments can help.
Posted May 23, 2019 Reviewed by Lybi Ma
Most people consider chronic pain—such as pain that lasts for months or years from a bad back or arthritis—a medical condition that should be treated exclusively by a physician or physical therapist. Although this view of chronic pain is common, it is often incorrect—and has resulted in much unintended harm, particularly in recent years. In this post, we’ll learn how a simple medical model for chronic pain frequently produces disappointing treatment results and examine an alternative model for chronic pain based on the best available pain research that reduces harms while improving results.
How people think about chronic pain is important for two reasons. One reason is that chronic pain is one of the most common types of health problems among U.S. adults. Statistics from the Center for Disease Control, for example, indicate that chronic pain affects 1 in 5 (20 percent) of adults. This translates to more than 50 million Americans! Whatever becomes the consensus thinking about chronic pain, therefore, will influence a lot of people.
The second reason is that when people with chronic pain see their condition only as a medical problem, they run the risk of over-relying on medical treatments such as pain medicines and surgeries. Clearly, some patients with chronic pain obtain excellent results with medical treatments alone; however, many other patients either obtain limited improvements or even suffer harms such as surgical complications or addictions to pain medicines. The more a patient relies on medical approaches as their primary treatment for chronic pain symptoms, the higher their risk of experiencing these negative outcomes.
Based on more than a half-century of pain research, we now know that it is more accurate to think of chronic pain as being both a medical condition and a psychological condition. The psychological part of chronic pain refers to the degree of negative social, emotional, and quality of life effects experienced by a patient. In the same way that patients with chronic pain differ greatly in regards to how much the medical side of their condition affects them—one patient with chronic back pain may continue to work and maintain most of their social activities in modified form, for example, whereas another patient with chronic back pain may be unemployed and socially isolated—so too do patients vary in the degree to which they struggle with the psychosocial side of chronic pain. Research shows, for instance, that 33 to 50 percent of patients with chronic pain report clinically elevated levels of depression or anxiety.
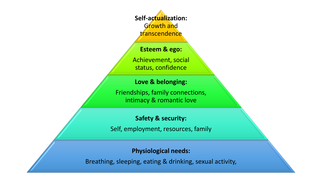
To appreciate the psychology of chronic pain, it is useful to refer to a classic psychological theory called Maslow’s hierarchy of needs. Shown in the left figure, psychologist Abraham Maslow believed that human motivation could be understood in terms of innate drives to fulfill physical, social, intellectual, emotional, and spiritual needs. He also believed that these needs could be ordered from basic needs shared across animal life—such as safety—to the highest-level, human-only need he called self-actualization. In Maslow’s model, psychological pain and emotional suffering resulted when people were unable to find ways to fulfill their human needs or when they become trapped in a low-level need and unable to grow (e.g., financial stress causing a person to struggle to meet basic housing and security needs or a divorce producing depression by disrupting important social and emotional needs).
Chronic pain is a rare condition with the ability to disrupt ALL levels of Maslow’s hierarchy. Beyond the unpleasant experience of pain itself, consider some of the ways that chronic pain affects our human needs:
- Pain limits our ability to maintain our family roles as breadwinners, parents, and spouses. Guilt is a common experience among patients with chronic pain when they feel inadequate as parents or romantic partners.
- Pain increases our dependence on others. Over time, many patients with chronic pain come to feel like burdens.
- Pain creates uncertainty about the future, upsetting financial stability and future goals. Anxiety and fear are the most common emotional responses to chronic pain.
- Pain harms relationships with family, friends, and work. Patients with chronic pain frequently become isolated and disconnected from others.
- Pain often steals sources of happiness, contribution, and achievement as a patient’s ability to engage in hobbies, work, and recreational activities is reduced.
The result is that chronic pain adds many sources of stress—while simultaneously subtracting many of our sources of reward and meaning.
Because chronic pain includes a medical side and a psychological side, many patients with chronic pain benefit from including a pain psychologist as part of their treatment program. Patients often react to a pain psychology recommendation as a threat, believing that pain psychology is for patients whose pain is “in their heads.” However, this is simply not true. Pain psychology treatments are potentially useful for every patient with chronic pain. This is because pain psychology aims to help each patient address the ways in which their pain condition is interfering with their ability to fulfill their human needs, using many different treatment approaches to restore relationships and improve function, meaning, contribution, and sources of personal growth.
LinkedIn Image Credit: Roman Samborskyi/Shutterstock


